If you have diabetes, engaging in diabetic foot care is essential. Patients with diabetes are more likely to have foot problems, as diabetes can damage your nerves and lessen blood flow to your feet.
Diabetic foot care is all about maintaining the health of your feet and being aware of the particular challenges diabetes can pose for your feet.
How Diabetes Impacts Your Feet
Diabetes is about more than just balancing your blood sugar. Diabetes is a systemic disease that impacts all body systems. It can restrict blood flow to your feet.
This results in decreased nerve sensation in your feet, which can lead to delays in recognizing injuries to your feet. Decreased nerve sensation can also cause cuts and blisters to take longer to heal, increasing the chance of a wound developing.
Common Diabetic Foot Problems
Specific foot problems commonly occur in diabetics. This can include bunions, hammertoe, ingrown toenails, corns and calluses, and foot ulcers. If foot issues are left untreated, potential infections or foot wounds can develop.
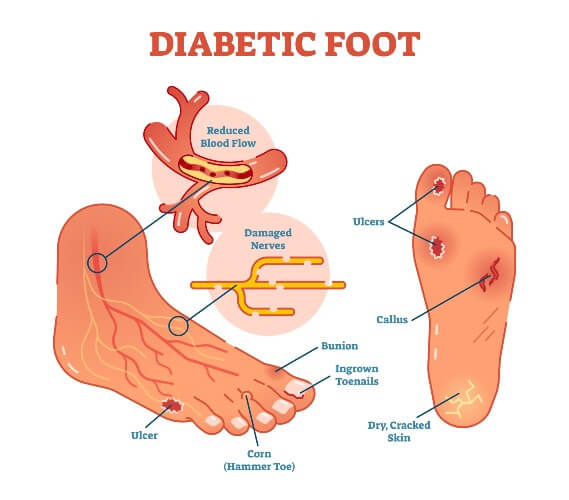
Why Infections and Foot Wounds are Common for Diabetics
One of the side effects of diabetes is poor circulation, which can lead to loss of feeling in the feet. When you lose sensation, you may not be aware when you injure your foot, allowing the injury to linger and resulting in an infection.
When you have high blood sugar, the walls of the blood capillaries that supply oxygen and nutrition to the nerves can weaken. Weakened capillaries can result in nerve damage and loss of sensation.
Weekend capillaries most impact your feet because they are the part of your body that is furthest from your heart.
This condition is known as diabetic neuropathy. Diabetic neuropathy most often impacts the nerves in the legs and feet. It can result in pain and numbness in the feet, legs, and hands.
Diabetic neuropathy can make your skin dry and crack easily, allowing infection-causing bacteria to enter your skin. This is one of the reasons diabetic patients suffer from more foot wounds like ulcers.
Severe infections can occur when cracked skin and other minor wounds are left untreated. These infections can be more complicated to treat due to poor blood circulation, which makes it harder for the blood to deliver antibiotics to the wound site. All of this combines to make diabetic wounds challenging to heal.
Preventative Foot Care to Avoid Complications
For diabetic patients, preventative foot care is critical. At Advanced Foot & Ankle Wellness Center, we recommend patients with diabetes implement preventative foot care measures to avoid serious foot complications.
- Inspect feet daily: Take a few minutes daily to inspect your feet for any wounds. Be on the lookout for redness, blisters, bruising, warm areas, and nail problems. Are you having a hard time inspecting the back of your foot? Use a mirror!
- Never walk barefoot: Diabetic nerve damage reduces your ability to detect cold and hot surfaces with your feet and can significantly reduce your ability to feel pain. That is why you shouldn’t walk around barefoot, inside or outside. Wear slippers or indoor shoes inside, and always put on safe footwear when you go out. This will reduce your risk of injury and infection.
- Clean your feet daily: Don’t forget to clean your feet daily. When you bathe, wash your feet with warm water and mild soap. Carefully pat your feet dry to get rid of all moisture. Don’t soak your feet; that can dry out your skin.
Carefully moisturize your feet: Apply unscented lotions to your feet to prevent dry skin. Don’t apply lotion between your toes, though, as extra moisture in that area can lead to an infection. - Wear socks: At night, when you sleep, wear socks to keep your feet warm. In cold weather, always put on socks as well. You may not be able to tell when your feet are cold with diabetic neuropathy, which is why you need to be more careful about wearing socks.
- Quit smoking: If you smoke, stop immediately. Smoking damages blood cells, and if you already have poor blood circulation and diabetic nerve damage, that can further increase your risk of foot infection and amputation.
Wear comfortable shoes: Wear shoes that fit and are comfortable. Avoid shoes that are too small or too tight. Avoid shoes with pointed toes and high heels. Make sure the shoes you wear fully support your feet. Custom orthotics and custom footwear provide relief from neuropathy and vascular issues.
These tips are great ways to take care of your feet and prevent injuries and wounds from appearing.
Common Complications Linked to Diabetic Foot Wounds
If you suffer from an infection as a diabetic patient, you should get treatment as soon as possible to avoid complications. Even what appears to be a very small wound visually can lead to a severe infection.
Diabetic Foot Ulcers
A diabetic foot ulcer is an open sore or wound on the foot. It is usually located on the bottom of the foot.
Foot ulcers can be dangerous, especially if they go untreated for too long. They can lead to significant infection and possible amputation if not treated.
With a diabetic foot ulcer, the treatment depends on the severity of the ulcer. The wound may need to be cleaned by a doctor, and any dead or infected tissue removed. Antibiotics may need to be administered to eliminate the infection. In some cases, a vascular surgery evaluation may be required.
People with other diabetes-related diseases that impact the kidney, eyes, and heart are at a greater risk of developing a foot ulcer. Individuals who use insulin are at a greater risk as well. Other risk factors include regular alcohol and tobacco usage and being overweight.
If you have diabetes and develop a foot wound, please schedule follow-up care with Advanced Foot & Ankle Wellness Center as soon as possible.
Foot Amputations
Amputation may be necessary if you get a foot infection that doesn’t clear up after debridement, where all the dead and infected tissue is removed, or after being treated with antibiotics.
Foot amputations are a common complication for diabetic patients with neuropathy. That is why proper care to avoid foot amputation is essential.
At Advanced Foot & Ankle Wellness Center, Dr. Melissa Wawrzynek will work with you to provide alternatives to surgery.
When to See Your Doctor
- As a patient with diabetes, you need to take special care of your feet. If you experience any of the symptoms below, schedule an appointment with Advanced Foot & Ankle Wellness Center:
- Dry, cracking skin on your foot
- Yellow and thickening toenails
- Fungus infection between your toes
- Ingrown toenail
- Infected corn
- Blister, sore, or ulcer
- Loss of hair on toes, feet, and lower legs
- Change in the shape of your feet
- Loss of sense of touch in your feet
- Loss of the ability to feel heat or cold in your feet
- Pain
- Tingling or burning sensation
- Change in the color or temperature of your feet
Most individuals with diabetes can prevent serious foot complications with regular preventative foot care at home, proper diabetes management, and working closely with their doctor at Advanced Foot & Ankle Wellness Center to take care of their feet.
Dr. Melissa Will Help Get You Back On Your Feet
Dr. Melissa Wawrzynek is a board-certified foot and ankle specialist and offers a broad range of advanced orthopedic, sports medicine, and regenerative treatments.
Our doctor and her team will consult with you regularly to ensure you return to health and receive the highest quality care.
If you’re ready to return to full speed as quickly, easily, and safely as possible, schedule an appointment today.

